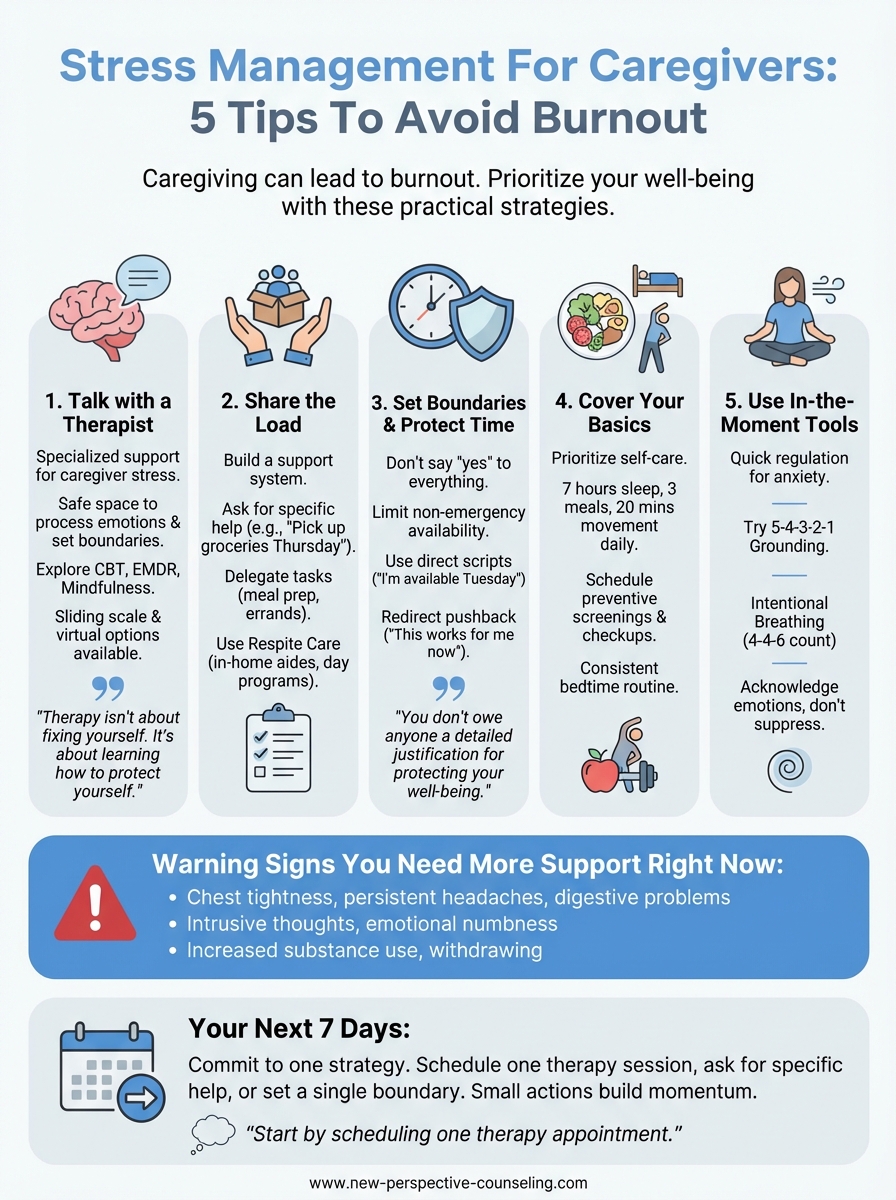
Stress Management For Caregivers: 5 Tips To Avoid Burnout
Caring for a loved one with a chronic illness, disability, or age-related needs can be one of the most meaningful roles you’ll ever take on, and one of the most exhausting. Between medical appointments, daily tasks, and emotional support, your own needs often get pushed aside. Without intentional stress management for caregivers, the physical and emotional toll can quietly build into something more serious: burnout.
Burnout doesn’t happen overnight. It creeps in through sleepless nights, mounting frustration, and the slow erosion of your own identity outside of caregiving. You might notice you’re more irritable, less patient, or completely drained before your day even begins.
At New Perspective Counseling, we work with individuals navigating the pressures of caregiving and other significant life challenges. This article offers five practical strategies to help you protect your well-being while continuing to show up for the people who depend on you.
1. Talk with a therapist who understands caregiver burnout
Working with a therapist who specializes in caregiver stress gives you a safe space to process emotions you might not feel comfortable sharing with family or friends. Many caregivers push through exhaustion and resentment without realizing how deeply it affects their mental and physical health. A trained clinician can help you identify patterns, set realistic boundaries, and develop coping strategies that fit your specific caregiving situation.
Therapy isn’t about fixing yourself. It’s about learning how to protect yourself while you’re carrying so much.
What to bring to your first session
You don’t need a formal list, but walking in with a few key details can help your therapist understand your situation faster. Share how long you’ve been caregiving, what your daily responsibilities look like, and what feels most overwhelming right now. Mention if you’ve noticed changes in your mood, sleep, or physical health. If you’re experiencing guilt, anger, or grief about your role, name that too. Therapists who work with caregivers recognize these feelings as normal responses to chronic stress, not personal failures.
What therapy can help you change fast
Therapists use approaches like Cognitive Behavioral Therapy (CBT) to help you challenge unhelpful thought patterns and Eye Movement Desensitization and Reprocessing (EMDR) or Brainspotting to process trauma or distressing memories related to caregiving. You might also explore mindfulness techniques that reduce reactivity in high-stress moments. Many clients notice shifts in how they respond to difficult situations within just a few sessions, especially when they practice skills between appointments.
What to do if time and cost feel impossible
Most therapists offer evening or weekend appointments, and many now provide virtual sessions that eliminate travel time. If cost is a concern, ask about sliding scale fees or whether your therapist accepts insurance. Some community mental health centers and nonprofit organizations offer low-cost counseling specifically for caregivers. Even one session per month can give you the support and tools you need to manage stress more effectively when daily demands feel relentless.
2. Share the load with a clear support plan
Caregiving doesn’t have to be a solo mission, even when it feels like you’re the only person who knows how things need to be done. Building a structured support system reduces the pressure on you and helps the people in your life contribute in meaningful ways. Effective stress management for caregivers often starts with asking for specific help and creating a schedule that distributes responsibilities before you reach your breaking point.
How to ask for help without feeling guilty
You can make clear requests by naming the exact task and timeframe. Instead of saying “I need help,” try “Could you pick up groceries on Thursday afternoons?” or “Can you sit with Mom every Tuesday evening so I can go to therapy?” Specific asks make it easier for others to say yes and follow through. Many caregivers worry they’re burdening others, but your loved ones often want to help and just don’t know where to start.
People can’t support you if they don’t know what you need.
What to delegate and what to keep
Consider handing off tasks like meal prep, transportation to appointments, errands, bill paying, or light housekeeping. Keep the responsibilities that require your specific knowledge or involve medical decisions only you can make. Write down everything you do in a week, then identify three to five tasks someone else could handle with minimal instruction.
How to use respite care before you hit a wall
Respite care provides temporary relief through in-home aides, adult day programs, or short-term facility stays. Look into local resources through your state’s aging and disability services or healthcare provider. Schedule respite care regularly, not just during emergencies, so you can rest and recharge before exhaustion becomes dangerous.
3. Set boundaries and protect your time
Saying yes to every request drains your energy and makes effective stress management for caregivers nearly impossible. Without clear boundaries around your time and availability, you’ll constantly operate in crisis mode, responding to everyone else’s needs while ignoring your own. Setting limits isn’t selfish. It’s how you sustain your ability to care for others without sacrificing your physical and mental health in the process.
Where caregivers overcommit most often
You probably overextend yourself in situations where guilt drives your decisions more than practicality. Common traps include saying yes to every family gathering, handling all communication with medical providers, managing finances for multiple households, and being available 24/7 for non-emergency situations. Many caregivers also commit to volunteering at their care recipient’s facility or coordinating care for other family members beyond their primary responsibility.
Scripts to say no and reset expectations
Try these direct responses: “I can’t make that appointment work, but I’m available Tuesday morning instead.” “I need to leave by 6 PM on weekdays. Let’s find someone else to cover evenings.” “I’m not checking messages after 9 PM anymore. I’ll respond in the morning.” Start sentences with “I’ve decided” or “I need to” rather than apologizing or over-explaining your choices.
You don’t owe anyone a detailed justification for protecting your well-being.
How to handle pushback from family and providers
Expect resistance when you first establish limits, especially from people accustomed to your constant availability. Stay consistent with your new boundaries even when others express frustration or disappointment. Redirect pushback by saying, “This is what works for me now” or “I need to make this change to continue providing care long-term.” If healthcare providers schedule appointments outside your stated availability, ask them to find alternative times or coordinate with another family member you’ve designated.
4. Cover your basics like sleep, food, movement, and care
Your body can’t run on fumes indefinitely. When you skip meals, ignore symptoms, or push through exhaustion, you compromise your ability to provide quality care and increase your risk of serious health problems. Prioritizing basic self-care isn’t optional. It’s a non-negotiable part of sustainable stress management for caregivers that protects both you and the person depending on you.
A realistic self-care minimum for busy caregivers
Start with what you can actually maintain: three simple meals daily, 20 minutes of movement (even walking counts), and seven hours of sleep most nights. You don’t need expensive gym memberships or elaborate meal prep. Keep grab-and-go protein options like nuts, cheese, or hard-boiled eggs within reach. Stretch during commercial breaks or while your loved one rests. Build movement into existing activities like parking farther away or taking stairs when possible.
How to improve sleep when nights feel unpredictable
Create a consistent bedtime routine even when interruptions happen. Set your bedroom 10 degrees cooler than the rest of your home and block out light completely. If you wake during night shifts, take 20-minute power naps during daylight hours rather than trying to function on zero sleep. Consider a baby monitor or alert system that lets you hear emergencies without staying awake all night listening.
Your body needs rest to repair itself and maintain the energy caregiving demands.
How to stay on top of your own medical needs
Schedule your annual checkups and preventive screenings six months in advance, treating them as immovable appointments. Keep a running list of symptoms or concerns to discuss with your doctor so you don’t minimize issues during rushed visits. Ask your physician about medication delivery services and telehealth options that eliminate travel time.
5. Use in-the-moment tools to calm your nervous system
You can’t always control when stress hits, but you can control how you respond to it. Learning quick regulation techniques gives you practical ways to manage anxiety, frustration, and overwhelm without leaving your caregiving responsibilities. These tools activate your body’s calming mechanisms and help you reset when tension builds throughout your day.
Quick grounding and breathing techniques you can do anywhere
Try the 5-4-3-2-1 method when you feel overwhelmed: name five things you see, four you can touch, three you hear, two you smell, and one you taste. This pulls your focus from racing thoughts back to your immediate environment. For breathing, inhale slowly through your nose for four counts, hold for four, exhale through your mouth for six. The longer exhale signals your nervous system to shift out of stress mode.
Even two minutes of intentional breathing can break the cycle of mounting tension.
How to stop the spiral of worry and resentment
When negative thoughts loop, write them down instead of letting them cycle endlessly in your head. Seeing your worries on paper often reveals they’re less catastrophic than they feel. For resentment, acknowledge it without judgment, then redirect your focus to one specific thing you can control right now. Effective stress management for caregivers includes accepting difficult emotions rather than suppressing them.
Warning signs you need more support right now
Watch for physical symptoms like chest tightness, persistent headaches, or digestive problems that won’t resolve. Notice if you’re having intrusive thoughts about harm coming to yourself or your loved one, or if you feel emotionally numb instead of connected. Increased substance use, withdrawing from relationships, or fantasizing about running away all signal you need professional intervention immediately.
Your next 7 days
Pick one strategy from this article and commit to it for the next week. You don’t need to overhaul your entire routine overnight. Start by scheduling one therapy appointment, asking one person for specific help, or setting a single boundary that protects your most exhausted hours. Small, consistent actions create momentum that builds sustainable stress management for caregivers over time.
Your next seven days might include blocking off Tuesday evenings as non-negotiable personal time, delegating Saturday grocery runs to a family member, or practicing three minutes of breathing exercises each morning before your loved one wakes. Write down which strategy you’ll implement and what success looks like by next Monday. Track how you feel physically and emotionally as you make this one change.
Professional support makes every other strategy more effective. At New Perspective Counseling, our therapists understand the specific pressures caregivers face and can help you build a personalized plan that protects your well-being while you continue showing up for others. You don’t have to wait until you’re completely burned out to ask for help.